
Related articles


eCOA vs ePRO: Understanding the differences in clinical trials
Digital data capture has become essential to modern clinical research. Sponsors and research organizations increasingly rely on electronic outcome assessment tools to collect high quality patient data, reduce manual errors, and improve regulatory compliance.
Two terms appear frequently in this space: eCOA (electronic Clinical Outcome Assessment) and ePRO (electronic Patient Reported Outcome).
These terms are closely related. However, they are not interchangeable.


eCOA standards and KPIs to include in your next RFI
According to Gartner, a request for information, or a request for proposal, is defined as “both the process and documentation used in soliciting bids for potential business or IT solutions required by an enterprise or government agency. The RFI document typically outlines a statement of requirements (SOR) to be met by prospective respondents wishing to make a bid to deliver the required solutions. It might cover products and/or services to meet the given requirements.”
Yet, for anyone entering into a long-term business agreement, a well-written RFI can do so much more than just assess and collect vendor capabilities.
For the last decade, Medable has been transforming the capabilities of organizations across clinical research using the latest in new technologies. In this time, we’ve learned the best RFIs are able to define what success looks like, create alignment on measurable outcomes, and establish accountability on roles and responsibilities well before a contract is ever signed. When done correctly, it becomes a decision-making framework that offers clear vision to both organizations.
Recently, Medable received two RFIs around eCOA from top pharmaceutical organizations. They stood out to us because they were structured around performance, not promises, a distinction that makes all the difference.
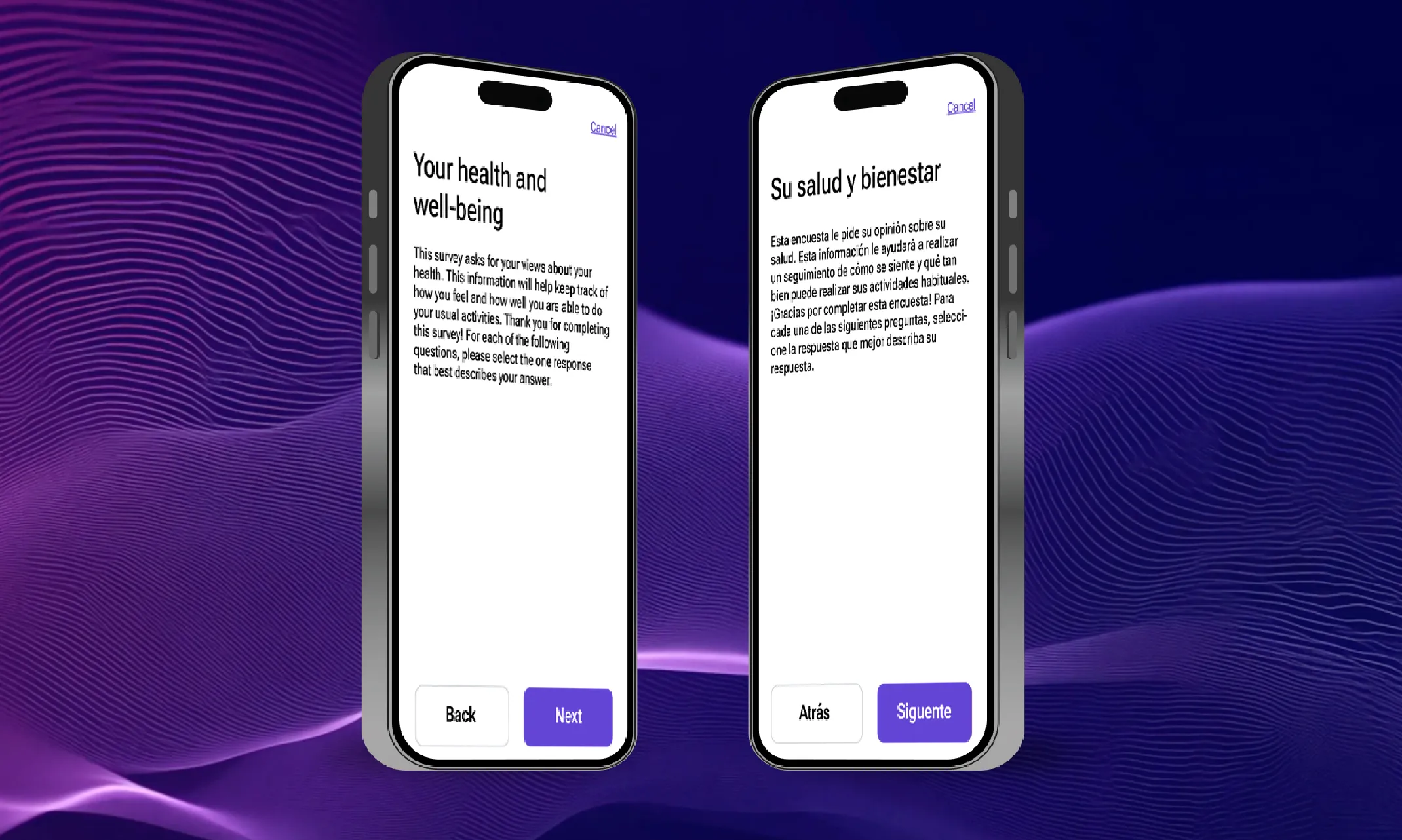

From bottlenecks to breakthroughs: How AI is transforming translation timelines
According to ClinicalTrials.gov, there are 3,046 multi-country trials being conducted this year. While many trials remain localized within a single country, there has been a definitive movement towards conducting trials in multiple countries, especially for larger, later-stage trials. This is driven by the positives that multi-country trials offer, like faster patient recruitment, lower costs in some regions, and the need for diverse patient populations.. However, behind the scenes, a critical bottleneck has been slowing many trials down. This bottleneck is the translation process that’s required to make trials work across multiple languages, locales, and regulatory bodies/organizations.




